Treating Clients with Primary Progressive Aphasia: 7 Tips for the Speech-Language Pathologist
9 min read
You may feel comfortable treating clients with dementia as well as those with aphasia after a stroke, but what about clients with primary progressive aphasia? Primary progressive aphasia (PPA) is a relatively rare, and often under-diagnosed, neurological disorder that primarily affects language and the person’s ability to communicate. Although similar in many ways to dementia or aphasia following a stroke, PPA is a unique progressive condition requiring its own approach to assessment and treatment.
Learn more about primary progressive aphasia and the various types of PPA.
PPA is different from the more typical presentation of dementia. With Alzheimer’s dementia, memory loss is one of the first signs. With PPA, difficulty with language is the first sign, while memory and reasoning are usually not affected in the early stages. When helping clients with aphasia after a stroke, you expect to see improvements as they recover. Clients with PPA have a degenerative disease that gets worse as time goes on. So what can an SLP do? Plenty!
Tips for Treating Primary Progressive Aphasia
As with any new client or condition, assessment is the first step in the therapeutic process. Meet the client where they are, and learn about the individual to get a picture of their strengths and weaknesses for both language and non-linguistic skills. Listen to them and their caregivers.
- What is important to them?
- What are their questions, concerns, and frustrations?
- What are they doing that is working?

Understand that every person progresses differently. Each of the three subtypes of PPA has a different presentation, so it’s important to know what you’re dealing with. Complete your favorite aphasia assessment (e.g. Western Aphasia Battery, Aphasia Diagnostic Profiles, Boston Diagnostic Aphasia Examination) to get a comprehensive picture of their aphasia. The Cognitive-Linguistic Quick Test + (CLQT+) is adapted for people with aphasia and will help assess cognition along with language.
When choosing standardized tests to help you assess and measure progress for a client with PPA, it’s best to prioritize their functional needs to enhance their quality of life. As language skills may not improve during treatment, improving function is where you will see the most progress and benefit from your treatment. Assessments that focus more on function include:
- Communication Activities of Daily Living – 3rd edition (CADL-3)
- Assessment for Living with Aphasia (ALA)
- Quality of Communication Life Scale (ASHA QCL)
- American Speech-Language-Hearing Association Functional Assessment of Communication Skills for Adults (ASHA FACS)
Since your treatment focus will be on increasing your client’s level of function, you’ll need to focus on preserving strengths and compensating for weaknesses. Use the client’s personal priorities when setting measurable goals, determining treatment tasks, and making a plan for the future.
Early Stages of Primary Progressive Aphasia
The early stages of PPA often present similarly to post-stroke aphasia. Memory and reasoning are usually not affected in the early stages. The person’s intellect and memory will be relatively normal, but their comprehension or expressive communication will be impacted. You will want to evaluate similar to a post-stroke aphasia, though treatment will be very different. Focus on maximizing function and planning for the future.
Mid to Late Stages of Primary Progressive Aphasia
Later stages of PPA may present similarly to dementia, though the distinction is important. With dementia, memory loss and other cognitive programs are one of the first signs. With PPA, language is the early sign and will be impacted more severely, so try to assess memory and judgment separately from language as best you can. As PPA progresses, language will worsen and other symptoms will appear, depending on the type of PPA. For example, people with PPA-nonfluent subtype may develop more executive function problems, dysphagia, and motor/dexterity problems. People with PPA-semantic subtype may show more changes in behavior and personality and have difficulty recognizing objects and faces.
Tips for Treating Primary Progressive Aphasia
1) Practice Priority Vocabulary
With PPA, don’t expect the same carryover of skills as you would when treating a stroke survivor with aphasia. The brain isn’t learning the same way, so working on one set of words is unlikely to carry over and show gains on a different set. Practice only what’s important to your client. For example, if the client loves pineapple, then use the word in your program. If they don’t care for or need to talk about pineapple, then leave the word out of treatment.
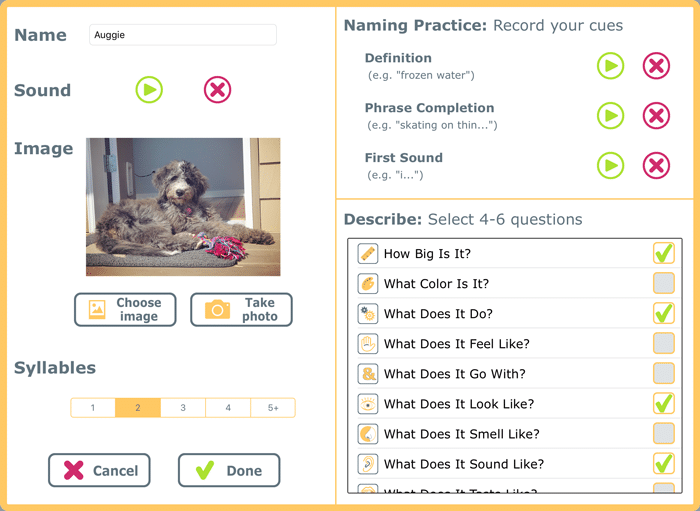
In the Language Therapy apps, you can add the people, places, and things that matter most to the person with aphasia or PPA.
Many apps are excellent to assist with traditional aphasia treatment, but may not be specific enough for your individual client and their priorities. Apps like Language Therapy allow you to enter custom word lists, so you can set up a home practice program with only words that are priorities for the client. The client can then practice naming, understanding, describing, reading, and writing to strengthen the words that matter to them.
Create opportunities for your client to practice important words and phrases. For example, you can create practice cards of family members, friends, and other important colleagues. To do this, place a person’s photo on one side of a card, then write their name and the most important information about them on the reverse side. The client can then practice looking at the photo and saying aloud as much as they can about the person. If they get stuck, they can peek at the back of the card. Set up the same exercise for their favorite restaurants or other locations. On the front, use a photo of the restaurant; on the back, include the restaurant name, town, and their favorite dish when eating there.
2) Teach Scripts for Primary Progressive Aphasia
If it’s early in the progression of primary progressive aphasia, have the family and the client pay attention to routines and phrases used in everyday life. Ask a family member to write them down. Now you will have a list of what is important to the client’s everyday life, and these phrases can be used as scripts to practice as the PPA progresses.
What is a script and how do I do it? Check out this article on Developing and Using Scripts in the Treatment of Aphasia, Apraxia of Speech and TBI from Audrey Holland, Ph.D.
Speaking scripts can be used for:
- Typical conversations
- Ordering in a restaurant
- Routine phone calls
While written scripts/models can be used for:
- Texts
- Check-writing
Tips for effective scripts:
- Vary the number and complexity of the scripts based on the stage of PPA – the more severe the PPA, the fewer and simpler the scripts.
- Use the individual’s phrasing as much as possible.
- Focus on clarity and minimizing frustration. When in doubt, simplify the script – you aren’t trying to teach something new, you are strengthening and compensating.
- Prioritize based on what’s important to the client.
3) Train Compensatory Strategies for Primary Progressive Aphasia
As you do with aphasia or dementia, identifying and using communication strengths can help you determine effective compensatory strategies, as well as build confidence. Modify interests and activities so they are easier and the person can compensate for language problems. Sometimes it’s as simple as labeling items in the environment.
Clients should practice using strategies, alternative communication, and scripts in comfortable situations with the SLP, their family, and close friends. This will make it easier to use them in public.
Case Example:
I treated a client with word-finding problems as well as decreased auditory comprehension. He reported he has always been an avid list-user, and we noticed he tended to pay attention to what he sees, rather than what he hears. I trained the client and his spouse to write keywords as they are conversing, including drawing pictures or using visuals to clarify what is being said. This helped both people to “be on the same page.”
4) Create a PPA Business Card
Clients who are still independent in the community may benefit from carrying an individualized information card. This card can be shown to others to communicate that the person has aphasia, which strategies can help, and a person to contact in emergencies. This can be useful if the person struggles at the grocery store or library, or if they have an interaction with the authorities. Cards can also be useful for other compensatory approaches, such as a script for ordering a cup of coffee or checking in for a tee time.

Make sure the card is easily accessible by the client in a familiar location, like in their wallet or purse, next to their driver’s license or photo ID. The card should include whatever information the person is comfortable sharing that would be helpful including:
- Name
- Explanation of the communication difficulty or diagnosis (consider including that they are not drunk or on drugs, as is often assumed)
- Quick communication tip strategy that can help (e.g. “use short phrases”, “speak slowly”, “allow extra time to understand”, “be patient”)
- Emergency contact person’s name and phone number
5) Train Nonverbal Communication
As PPA progresses and communication skills (especially verbal skills) decline, nonverbal skills become that much more important. Nonverbal communication is often more easily understood and produced. Teach care partners how to use and pay attention to gestures, eye contact, and body language. Have them write keywords, use visuals (pictures, drawings, objects), allow for extra thinking time, simplify their sentences, etc.
Learn to use supported conversation strategies with the free online SCA training from the Aphasia Institute.
6) Voice Banking and AAC
Many people choose to preserve their loved one’s voice by voice banking. If you choose an augmentative and alternative communication (AAC) device early enough, you can often record the client’s own voice saying the words/phrases when you program the device. Families may also want to consider recording videos of their loved one telling their favorite stories, singing or whistling a song they like to sing, or reading a book to their grandchildren. A free app called Marco Polo can be one way to do this; the app allows clients, their families, and friends to easily send short video messages to each other. The app saves the messages so you can look back and watch them whenever you like.
Care partners can also use AAC apps to help communicate their message when words fail. You can experiment with various AAC apps early on in treatment to see which app or style the client prefers, and begin customizing and training their use before they are needed.
7) Plan for the Future
Treatment should focus on a home program and compensatory strategies from the very first day. Set up routines and experiment with multimodal and alternative communication EARLY, even before the client really needs it. Early in the disease process, while more language and cognitive skills are still intact, it will be easier to understand and learn new techniques and routines. Earlier intervention gives clients and families time to become familiar with communication options, and time to decide what they like and what they don’t.
If possible, try to follow-up after discharge or check in with the client every few months. As PPA progresses and life changes, their home program and communication strategies will need to change as well.
A Final Word about Treating Primary Progressive Aphasia
The goal is effective communication, not perfection. Since PPA is a progressive disorder,
- early treatment,
- a personalized plan,
- partner training, and
- planning for the future
are important components of appropriate speech therapy treatment. Speech-language pathologists knowledgeable about PPA are uniquely qualified to assess the current impact on communication, identify priorities with the patient, and develop a treatment plan focused on compensatory strategies with a home program to preserve skills as long as possible.
We cannot stop PPA from progressing, but speech-language pathologists can help clients and families adjust their lives, compensate for their impairments, and keep the highest function and quality of life possible.
Continue your Learning about Primary Progressive Aphasia
- Many University research programs provide summaries of PPA, including the University of California- San Francisco and Northwestern.
- Read the ASHA Perspectives issues from SIG 2 October 2014 and SIG 15 May 2012 that focus on PPA.
- Where the Light Gets In: Losing My Mother Only to Find Her Again by Kimberly Williams-Paisley is a book about the author’s experience when her mother had PPA, offering insight into the care partner’s point of view.
- Watch and share this video about PPA from the National Aphasia Association.