A Day in the Life of an Acute Care SLP
7 min read
Brenda Arend shares highlights of a typical day for her as a SLP in an acute care hospital.
8:30 a.m. Assigning Patients
The first part of my day is spent opening up patient charts in our EPIC electronic medical record and assigning 3 SLPs to see the patients. I work at Providence St. Peter Hospital, a 380-bed hospital in Olympia, Washington. Two to three SLPs cover a caseload that ranges from 15 to 30 patients, though more recently we have seen as many as 42. In addition to our inpatient load, we also have an outpatient video fluoroscopic swallow study (VFSS) to do three days a week. Today I am assigned to see 7 patients and complete the outpatient VFSS.
9:00 a.m. Re-Evaluation in ICU
My first stop is in the intensive care unit (ICU) to see a man who had a heart attack. He aspirated secretions (meaning his saliva went into his lungs) during the cardiac arrest, and he had to be intubated (breathing tube) for 10 days. Another SLP assessed him yesterday and determined he was not ready to starting eating orally, so I’m there to re-assess. The patient pulled out his feeding tube yesterday, so the care team is eager to hear the results of my assessment.
While I’m with the patient, his alertness wavers, his cough is very weak when I ask him to clear his throat, and he is not managing his saliva well. I provide some oral care to clean his mouth and let the nurse know he’s still not ready to eat by mouth. I see in the chart he also has oral medications ordered, so I page the doctor to let her know it could be a few days before this patient is ready for oral intake. Now it’s up to her to decide if she wants to replace the feeding tube and change medications to non-oral administration. While I’m charting my findings, the radiology department calls to tell me the outpatient who was supposed to come in for the swallowing study has cancelled for today.

10:00 a.m. Swallowing Assessment
My next patient is a lady who had burr holes placed in her skull to remove a blood clot on her brain (a hematoma). She is awake, alert, has excellent oral control, and no signs of swallowing difficulty on my bedside evaluation. She looks great! I order a regular texture diet, write my chart note, and sign off.
10:52 a.m. Not Ready Yet
When I go to see my next patient, a man in his mid-30s who is in for street drug overdose, it’s clear he’s not alert enough for a swallowing evaluation today. I let the nurse know, and then spent 10 minutes talking to her about the nursing swallow screening we are trying to re-establish at my hospital. I love opportunities to provide education to nurses who have a genuine interest in what we do.
11:15 a.m. Upstairs to Oncology
This man has cancer at the base of his tongue, and a tracheostomy tube was placed in his throat to help him breathe. I’ve been following his case to evaluate his swallowing and make sure he can use a one-way speaking valve on his trach tube so he can speak audibly. Yesterday I did his video fluoroscopic swallow study (VFSS) using barium-infused food to see how it moves through his mouth and throat.
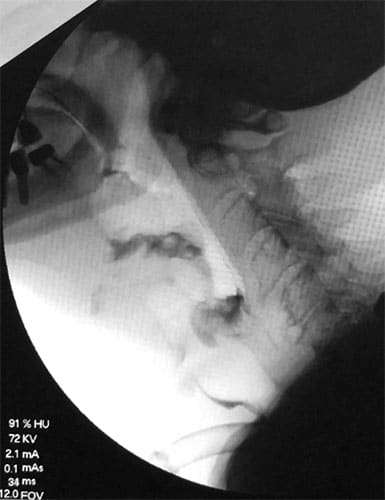
Today I’m teaching him swallowing exercises he can do during cancer treatment, even though he’ll be getting all his nutrition through a GJ feeding tube going directly into his intestines. I teach him the Mendelssohn maneuver, the Masako, and some range of motion exercises for his jaw. I’ll see him again in a week, after his radiation treatment has started.
The Dysphagia Therapy app, helps clinicians find the best therapy options for their patients based on assessment findings. Instructions, references, and anatomical information accompany each exercise in this indispensable pocket reference tool.
12:15 p.m. Lunch!
…and a meeting. While tucking into our lunch, the acute therapy team meets with the inpatient rehab screener twice a week. We share the names of patients we think will meet the requirements for the rehab program, as well as warn the screener of some who may not. I eat, talk to the other therapists, and play some Candy Crush for a much-needed mental break from the demands of the day.
1:15 p.m. Back to the Medical Floors
Or so I think! First radiology calls, notifying me of a new inpatient VFSS order. We schedule it for 2:30 that afternoon, giving me time to see the patient first so I know what to expect. I call the ordering medical doctor (MD) and ask for an additional order to see the patient at bedside prior to the VFSS.
1:30 p.m. Now, to the Medical Floors
I’m here to see a patient with dementia whom I saw yesterday for a swallowing assessment and placed on the baseline textures she was eating at her care facility (pureed solids and thin fluids). Today I check with nursing, read the chart, glance at the intake record, and observe her with the end of her lunch to find she is tolerating her baseline diet. I sign off.

2:00 p.m. Bedside Assessment
Remember that new VFSS order that came at the end of lunch? I go see the patient at his bedside and find him spitting out frothy secretions. He describes symptoms typical of an esophageal disorder, not oropharyngeal dysphagia (swallowing difficulty in the mouth or throat). Food feels stuck in the mid-sternal region, he has globus sensation (feeling of food sticking low in the throat), AND he has had two previous esophageal dilations where the connection between the esophagus and stomach are stretched to allow food to pass more easily.
I call the doctor to suggest we cancel the VFSS and get a consultation with the gastroenterologist (GI doctor) instead. The MD is grateful for my input and agrees to call for a SLP assessment again if this patient shows oropharyngeal dysphagia after the GI sees the patient. I call radiology to cancel the VFSS and write my note.
2:45 p.m. Stroke Treatment
I’m off to the neurology floor to see two patients who have had strokes; one with dysphagia and one with aphasia. With the dysphagia patient, I review the VFSS done yesterday, and with the information from that, I can plug the swallowing deficits seen during the test into my Dysphagia Therapy app to find some therapy strategies that target his particular deficits. I get hits for 4 different exercises, but today I just introduce one: the Chin Tuck Against Resistance (CTAR) exercise. I also have him practice using a tongue sweep to clear some mild pocketing of food in his cheek after small bites of crackers.
With the patient with aphasia, we work on saying numbers, days of the week, her husband’s name, and completing some basic phrases. She’s doing really well! This is exciting because yesterday she could not get out anything more than “yes” and “oh dear”.
Once stroke patients are ready for rehab, they get daily speech therapy focused on their communication. Read A Day in the Life of a Rehab SLP for more about what inpatient rehab might look like for a speech-language pathologist. Then ride along for A Day in the Life of a Home Health SLP to see what happens after patients go home.
4:00 p.m. Palliative Care
There is a new order on my screen, and since I’m through my list for the day, I pick up this new patient. A quick review of the chart tells me he is admitted with end-stage COPD (chronic obstructive pulmonary disease) and has orders for full comfort care (meaning no invasive treatments), but he also has an order for NPO – nothing by mouth. It’s time to take off my “rehab hat” and put on the “comfort care” hat. I enjoy the focus on quality of life when dealing with end of life care.
Fortunately, the patient’s daughter is in the room with him, and she expresses that she wants him to be able to eat and drink a little. After doing a brief bedside swallow evaluation, I explain the terms “comfort feeding” (just for pleasure, not nutrition) and “aspiration” (food or liquid entering the lungs), and we talk for a while to figure out what the right balance of risk and benefit will be for her dad. Basically, we want to find the least unsafe diet for him that still satisfies his desire to eat. We land on a pureed diet and sips of thin liquid, allowing him to have a few bites when he is alert enough to swallow. He is awake enough to agree and thanks me for the spoonfuls of ice cream I gave him earlier.
The next day I found out he passed away in the night, so those ice cream bites were the last food he ever ate. This makes me sad, but also grateful I was able to help.

5:00 p.m. Clock Out
Time to go home to my family. It was a day of great variety in patients and disorders. Each patient had complex medical issues that had to be considered in my work with them, which is what I think makes work in the acute setting a challenge, but also keeps it very interesting!



